Retronychia Definition, Symptoms, Causes, Treatment | Retronychia vs Paronychia
Retronychia is a proximal nail ingrowth that happens when the nail unit grows back into the proximal nail fold. Retronychia manifests clinically as persistent or chronic proximal paronychia with a disordered nail look, and it typically appears 3–6 months after a severe inflammatory or systemic disease. In some cases, retronychia is accompanied by onychomadesis, and in clinical settings, it might be mistaken for a nail tumor.
Retronychia can be detected on sonography by a noticeably decreased space between the origin of the nail plates and the base of the distal phalanx. It is possible to see thickening, decreased echogenicity, and varying degrees of ungual matrix thickening in the proximal nail fold, proximal nail bed, and surrounding tissue. This anomaly can also manifest as a complete or partial posterior embedding of the nail unit. It has been demonstrated that 3D ultrasonography can be helpful in the early diagnosis of retronychia as well as in improving clinical knowledge of the condition.
Definition
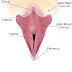
Retronychia is defined as the embedding of the nail plate into the proximal nail fold. Big toenails are the digits that are most frequently impacted.

Symptoms
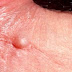
Retronychia is mostly caused by continuous microinjury to the nail, which is most commonly brought on by wearing shoes that are too tight or engaging in activities that can cause trauma to the toenail. Retronychia can be painful and show symptoms like xanthonychia, which is yellow or white staining of the nail plate, and inflammation of the proximal nail fold. The occurrence of xanthonychia and enlargement of the proximal nail folds instead of the lateral nail folds can assist distinguish retronychia from paronychia.
Causes
The most typical triggers include local trauma that puts pressure against the free edge and repeated small injuries (such as those caused by ill-fitting shoes or activities like jogging or hiking). Sometimes there are no triggers found. Systemic diseases like arthritis, thrombophlebitis as well as extreme stress episodes, might have an effect on the matrix region, which is often quite susceptible to hypoxia. These conditions have been described as potential causes of this phenomenon. Both reflex hypertension of halluces and lateral displacement of the big toe joint have been proposed as potential risk factors.
Studies using high-frequency ultrasonography revealed that retronychia is the consequence of a direct mechanism in which the entire nail section is embedded into the area of the proximal nail fold. In affected fingers, there is a smaller gap between the origin of the nail plates and the distal interphalangeal joint, demonstrating the retrograde motion, which is likely brought on by the development of traction pressures driven by scarring and inflammation.
Treatment
Retronychia is often treated by removing the infected nail from its bed at its proximal end. When viewed from the proximal side, the avulsed nail plate is enlarged and frequently has two or more layers. The surgery enables a speedy recovery and provides relief from pain. Early stages of the condition may benefit from conservative treatments such as taping, orthosis, and the local application of steroids. It is possible that up to 16% of cases will reoccur. It is uncommon to have permanent nail dystrophy after surgery.
 Reviewed by Simon Albert
on
October 12, 2022
Rating:
Reviewed by Simon Albert
on
October 12, 2022
Rating: